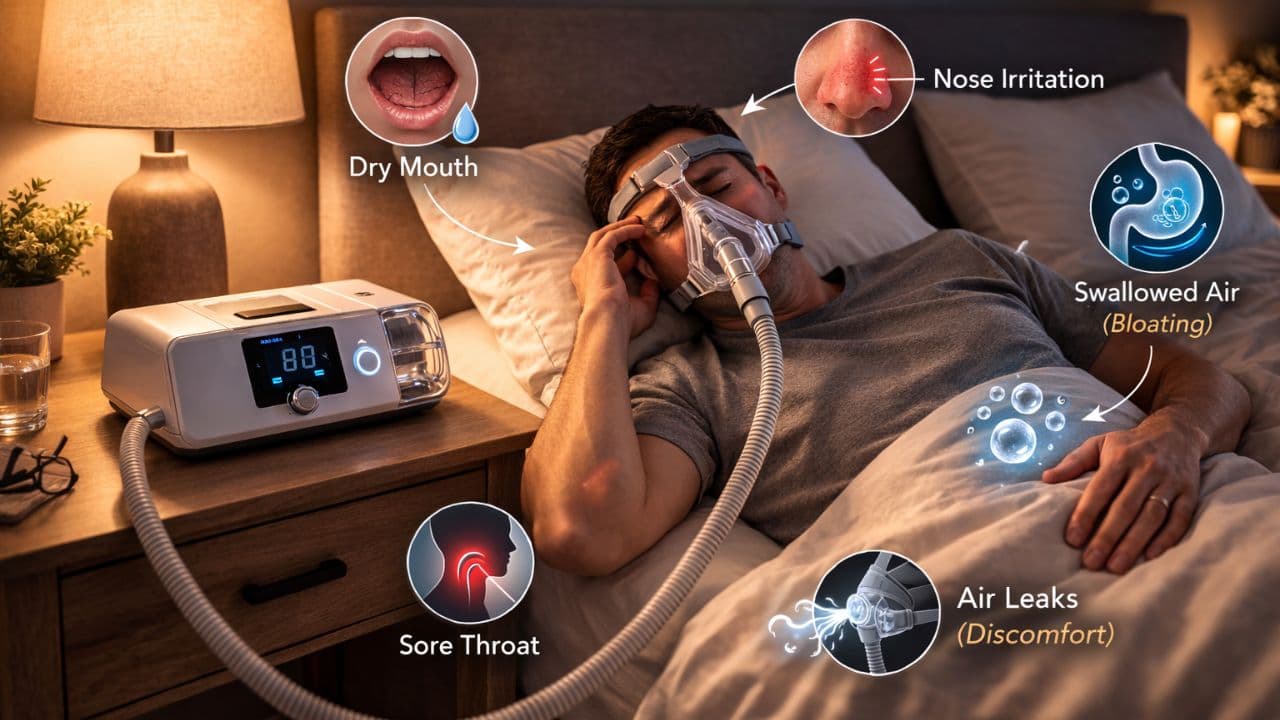
7 CPAP Side Effects and What to Do About Them
Dry mouth, mask leaks, skin irritation — CPAP side effects are real and they drive millions of patients to quit. Here are the most common problems and what you can do.
Reviewed by Dr. Andrew Gamache, DDS, D-IAOS
Last updated April 2025
Key Takeaways
- Up to 40% of CPAP users report chronic dry mouth, and 15-20% experience claustrophobia or anxiety from the mask.
- Most CPAP side effects have workarounds — but when multiple issues compound, they drive patients to quit treatment entirely.
- Oral appliance therapy eliminates mask-related side effects completely and has a 90%+ patient preference rate over CPAP.
1. Dry Mouth and Throat
Dry mouth is the single most common CPAP complaint. Pressurized air flowing through your nose and mouth all night strips away moisture, leaving you with a parched throat, cracked lips, and sometimes a sore tongue by morning. Studies show that up to 40% of CPAP users report chronic dryness as a persistent problem.
What you can do:
If dryness persists even with a humidifier, it may be a sign that your mask is leaking. Air escaping around the seal dries out your mouth and eyes simultaneously. A mask fitting appointment with your DME provider can help identify and correct leaks.
2. Mask Discomfort and Skin Irritation
CPAP masks press against your face for 6-8 hours every night. Over time, this constant pressure can cause red marks, skin irritation, pressure sores across the bridge of the nose, and even skin breakdown in severe cases. Many patients develop contact dermatitis from the silicone or latex materials.
Finding the right mask fit is critical, but many patients cycle through 3-5 different masks before finding one that is tolerable. Even then, seasonal changes in weight, facial hair growth, and skin conditions can affect fit over time.
What you can do:
3. Air Swallowing (Aerophagia)
Aerophagia — swallowing air — is one of the more uncomfortable CPAP side effects. The pressurized air meant for your lungs ends up in your stomach, causing bloating, gas, stomach distension, and belching. Some patients wake up with abdominal pain severe enough to be mistaken for a gastrointestinal problem.
This typically happens when CPAP pressure is set too high or when the patient mouth-breathes, creating a path for air to enter the esophagus. It can also worsen with certain sleeping positions.
What you can do:
4. Noise Disruption
Modern CPAP machines are significantly quieter than older models, but they are not silent. The motor produces a constant hum, and mask leaks create a whistling or hissing sound that often disturbs bed partners more than the snoring did. For light sleepers — both the patient and their partner — this noise can be enough to disrupt sleep quality.
Noise becomes a bigger issue in quiet environments. Patients who travel frequently also report difficulty using CPAP in hotel rooms where noise carries more easily.
What you can do:
5. Claustrophobia and Anxiety
For many patients, the sensation of wearing a mask strapped to their face with pressurized air blowing triggers feelings of claustrophobia or panic. This is not a minor inconvenience — it is a genuine psychological barrier that prevents effective treatment. Research suggests that 15-20% of CPAP patients experience significant anxiety related to the mask.
Some patients describe feeling trapped, suffocated, or unable to breathe naturally despite the machine delivering air. These feelings often worsen over time rather than improving, leading patients to remove the mask in the middle of the night or stop using it entirely.
What you can do:
6. Nasal Congestion and Nosebleeds
The continuous flow of pressurized air can irritate and inflame the nasal passages, causing chronic congestion, a runny nose, sneezing, and in some cases nosebleeds. Patients who already have allergies, deviated septums, or chronic sinusitis are particularly susceptible.
Ironically, nasal congestion often forces patients to breathe through their mouth, which makes other side effects like dry mouth worse and reduces CPAP effectiveness.
What you can do:
7. Relationship Strain
This is the side effect nobody talks about. The mask, the hose, the noise, and the overall appearance of CPAP can affect intimacy and self-image. Many patients feel embarrassed or self-conscious wearing the device around their partner. Some couples end up sleeping in separate bedrooms — not because of snoring, but because of the machine.
Partners may also feel frustrated by the disruption — dealing with mask leaks that spray air across the bed, the sound of the motor, or the tangle of hoses. While CPAP solves the medical problem, it can create new social and emotional ones.
The real impact: Sleep apnea patients who abandon CPAP due to relationship concerns are still at risk for the serious health consequences of untreated OSA. If CPAP is creating problems in your relationship, explore alternatives rather than going untreated.
When to Consider Alternatives
If you have tried adjusting your CPAP settings, switching masks, and working with your sleep physician but still cannot tolerate CPAP consistently, it may be time to consider an alternative treatment. The worst outcome is not switching treatments — it is abandoning treatment altogether and leaving your sleep apnea untreated.
Oral appliance therapy is the most common CPAP alternative. It is a custom-fitted mouthpiece — similar to a retainer — that holds your lower jaw slightly forward to keep your airway open during sleep. No mask, no hose, no electricity, no noise.
CPAP Side Effects
Oral Appliance Therapy
Not sure if you are a candidate for oral appliance therapy? Take our free 2-minute sleep assessment or learn more about how oral appliance therapy works.
Frequently Asked Questions
What is the most common CPAP side effect?
Dry mouth and throat is the single most common CPAP complaint, affecting up to 40% of users. A heated humidifier attachment can help, but many patients find the dryness persists — especially when mask leaks are present.
Can CPAP side effects go away over time?
Some side effects like initial mask discomfort may improve with adjustment. However, issues like claustrophobia, aerophagia, and relationship strain often persist or worsen over time rather than improving.
What can I do if I cannot tolerate my CPAP?
If you have tried adjusting settings, switching masks, and working with your sleep physician but still cannot tolerate CPAP, oral appliance therapy is the most common alternative. It is a custom-fitted mouthpiece with no mask, hose, or noise.
Does insurance cover CPAP alternatives?
Yes. Most medical insurance plans, Medicare, and TRICARE cover oral appliance therapy — especially when CPAP has been tried and failed. Your documented CPAP struggles actually strengthen the case for insurance approval.