Can You Have Sleep Apnea and Not Know It? Why 80% Go Undiagnosed
Most people with sleep apnea have no idea. The condition's most damaging events happen while you sleep, making self-detection nearly impossible. Here is why — and what to do about it.
Reviewed by Thomas D'Acquisto, Sleep Director, 39 Years in Sleep Medicine
Last updated February 2026
Key Takeaways
- Approximately 80% of people with moderate-to-severe sleep apnea are undiagnosed — the condition's signature events happen during sleep, making self-detection nearly impossible without a bed partner or sleep test.
- Many people normalize their symptoms for years, attributing chronic fatigue, morning headaches, and brain fog to stress, aging, or poor sleep habits rather than recognizing them as signs of a treatable medical condition.
- Women are disproportionately undiagnosed — an estimated 93% of women with moderate-to-severe OSA do not know they have it, partly because their symptoms overlap with conditions like depression and anxiety.
The Silent Condition
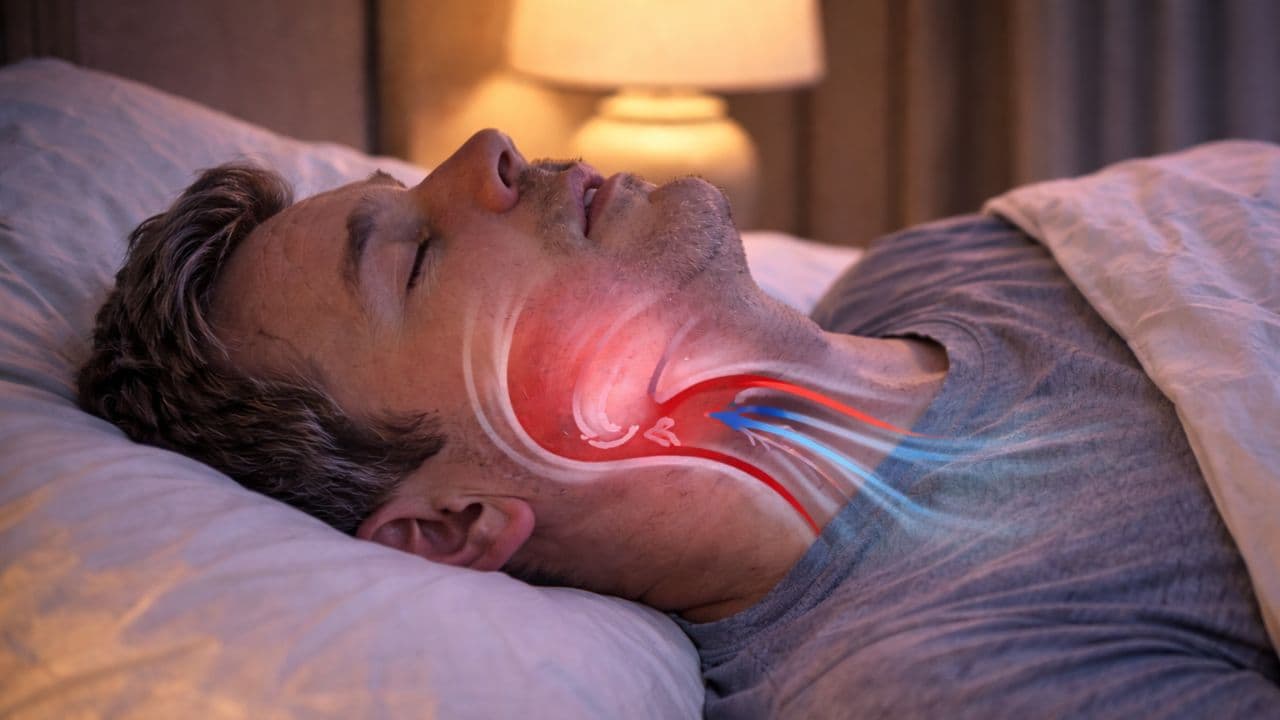
Sleep apnea is one of the most common medical conditions in the world — and one of the least diagnosed. The reason is deceptively simple: the condition's most harmful events happen while you are asleep. You cannot observe your own airway collapsing. You cannot feel the micro-arousals that fragment your sleep architecture. And by morning, the only evidence is a feeling you have learned to live with — exhaustion.
Americans Affected
Conservative estimate of US adults with obstructive sleep apnea — broader analyses suggest up to 83.7 million
Undiagnosed
Estimated percentage of moderate-to-severe cases that remain unidentified
Average Diagnostic Delay
Estimated time between symptom onset and diagnosis for the average patient
That 80% figure is not a rounding error. It means that for every person currently diagnosed and treated for sleep apnea, four more are living with it unaware. They are attributing their symptoms to stress, aging, depression, poor fitness, or simply "not being a morning person." The consequences compound silently — cardiovascular strain, metabolic disruption, cognitive decline — while the root cause goes unaddressed.
Why You Do Not Know You Have It
Sleep apnea avoids detection through several interlocking mechanisms. Understanding why it hides so well is the first step toward catching it.
You Cannot Observe Your Own Sleep
The defining events of sleep apnea — airway collapse, breathing cessation, oxygen drops, micro-arousals — all happen while you are unconscious. Each micro-arousal lasts only 3-15 seconds, too brief to reach waking memory. You may stop breathing 30 or more times per hour and have no recollection in the morning.
Symptoms Mimic Other Conditions
The daytime consequences of sleep apnea — fatigue, brain fog, mood disturbances, weight gain, headaches — overlap heavily with depression, hypothyroidism, chronic fatigue syndrome, menopause, and normal aging. Many patients receive treatment for these conditions for years before anyone investigates their breathing during sleep.
The Stereotype Excludes Most Patients
The popular image of sleep apnea is an overweight older man who snores like a freight train. While these are risk factors, sleep apnea affects women, fit individuals, young adults, and people who snore quietly or not at all. If you do not fit the stereotype, neither you nor your doctor may think to test for it.
Gradual Onset Prevents Recognition
Sleep apnea typically develops gradually over months or years. There is no sudden change that prompts alarm — instead, you slowly forget what feeling rested is like. By the time the fatigue is significant, you have already normalized it as part of who you are.
Solo Sleepers Lack a Witness
Bed partner observations — snoring, gasping, breathing pauses — are one of the most common pathways to diagnosis. People who sleep alone lose this early warning system entirely. Without someone to say "you stopped breathing last night," the condition remains invisible.
Signs You Might Be Missing
Even without knowing you have sleep apnea, your body gives clues. These signs often go unrecognized because they seem to have explanations — but when several occur together, they point toward a common cause.
Commonly Overlooked Signs of Sleep Apnea:
If three or more of these describe your regular experience, sleep apnea should be on your radar. Learn what sleep apnea actually feels like from the inside to understand how these symptoms connect to disrupted breathing during sleep.
Who Goes Undiagnosed the Longest
While anyone can have undiagnosed sleep apnea, certain groups face longer delays between symptom onset and diagnosis — often because their presentation does not match the clinical stereotype.
More Likely to Be Diagnosed:
Most Commonly Missed:
Women face a particularly severe diagnostic gap. While sleep apnea occurs in men only 2-3 times more frequently than in women, clinical diagnosis rates are skewed 8-10:1. Women with sleep apnea are more likely to present with fatigue, insomnia, and mood disturbances rather than the classic loud snoring — symptoms that lead to misdiagnosis as depression or hormonal imbalance. For a detailed look at this pattern, see our guide on signs of sleep apnea in women.
The Normalization Trap
Perhaps the most insidious reason sleep apnea goes undiagnosed is that you stop noticing how impaired you are. When fatigue develops gradually over months or years, you recalibrate your expectations downward. What was once "I feel terrible" becomes "this is just how I feel." You compensate — more coffee, earlier bedtimes, reduced activity — and assume the compensation is normal.
| What You Tell Yourself | What May Be Happening |
|---|---|
| "I'm just not a morning person" | Your brain never completes restorative sleep cycles, making mornings genuinely harder |
| "I need coffee to function — everyone does" | You are self-medicating a cumulative sleep debt that grows every night |
| "My memory is getting worse with age" | Chronic sleep fragmentation impairs memory consolidation regardless of age |
| "I'm just stressed and burnt out" | Sleep deprivation mimics burnout, and the two can compound each other |
| "I've always been a restless sleeper" | Restlessness may be your body fighting to find a position where the airway stays open |
The normalization trap is why so many patients, after starting treatment, describe a sense of revelation: "I forgot what it felt like to actually be rested." They did not realize how much they had lost because the decline was too gradual to notice.
How to Find Out for Sure
The only way to confirm or rule out sleep apnea is a sleep study that measures your breathing during sleep. The good news: this no longer requires a night in a hospital. Most patients can be diagnosed with a home sleep test — a portable device used in your own bed.
Take a Screening Assessment
A brief online questionnaire evaluates your risk based on symptoms, medical history, and physical characteristics. It takes under 2 minutes and helps determine whether a sleep test is appropriate for your situation.
Complete a Home Sleep Test
A compact, comfortable device is shipped to your home or picked up from your provider. You wear it for 1-2 nights while sleeping normally in your own bed. It measures airflow, blood oxygen levels, heart rate, and respiratory effort.
Receive Your Diagnosis
A board-certified sleep physician interprets your data and calculates your AHI (apnea-hypopnea index) — the number of breathing disruptions per hour. An AHI of 5 or above confirms sleep apnea, with severity classified as mild (5-14), moderate (15-29), or severe (30+).
Explore Treatment Options
If sleep apnea is confirmed, your provider discusses treatment options matched to your severity and preferences. Options include CPAP, oral appliance therapy, positional therapy, and combination approaches. Most patients begin to feel a difference within the first week of treatment.
For a detailed walkthrough, see our guide on what to expect from a home sleep test. Home sleep tests are covered by most PPO insurance plans, Medicare, and TRICARE.
Why Finding Out Matters
Undiagnosed sleep apnea is not simply "poor sleep." It is a progressive medical condition that places measurable stress on your cardiovascular, metabolic, and neurological systems every night. The longer it goes untreated, the more damage accumulates.
Cardiovascular Risk
Each apnea event triggers blood pressure spikes and oxygen drops. Over years, this leads to sustained hypertension, arrhythmias, and elevated risk of heart attack and stroke. Untreated severe OSA carries a 2.1x higher all-cause mortality risk.
Progressive Worsening
Sleep apnea is not static. Aging, weight changes, and hormonal shifts can worsen severity over time. A mild case today can become moderate or severe within a few years — increasing both symptoms and health consequences.
Cognitive Decline
Chronic sleep fragmentation impairs memory consolidation, executive function, and emotional regulation. Emerging research links untreated OSA to accelerated cognitive decline and increased Alzheimer's biomarkers.
The full picture of untreated sleep apnea's health consequences is sobering — but the critical takeaway is that treatment effectively reverses most of these risks. Patients who treat their sleep apnea consistently have mortality rates comparable to people without the condition.
Worth knowing: Treatment does not have to mean CPAP. For many patients — especially those with mild-to-moderate sleep apnea — a custom oral appliance is the preferred option. It is small, silent, portable, and achieves higher nightly adherence rates than CPAP for most patients.
If you suspect your sleep is not delivering the rest your body needs, the smartest move is the simplest: find out. Take our free 2-minute sleep assessment to evaluate your risk — no obligation, instant results.
Frequently Asked Questions
How long can you have sleep apnea without knowing?
Many people live with undiagnosed sleep apnea for years or even decades. The average delay from symptom onset to diagnosis is estimated at 5 to 7 years. During this time, the condition can progressively worsen and contribute to cardiovascular disease, metabolic problems, and cognitive decline.
Can a smartwatch or fitness tracker detect sleep apnea?
Some newer devices can detect potential signs of sleep apnea by monitoring blood oxygen levels and breathing patterns. However, these are screening tools, not diagnostic devices. A positive alert warrants a clinical sleep study, and a negative result does not rule out sleep apnea.
My partner doesn't say I snore — could I still have sleep apnea?
Yes. Not all sleep apnea patients snore loudly. Some experience only mild snoring, upper airway resistance, or silent apneas. Women in particular often present with fatigue and insomnia rather than prominent snoring. A sleep test is the only way to confirm or rule out sleep apnea regardless of snoring status.
What is the quickest way to find out if I have sleep apnea?
A home sleep test is the fastest path to diagnosis. After a brief screening assessment, a portable device is sent to your home. You wear it for one or two nights, and results are typically available within a few days. Many providers can complete the entire process — from screening to diagnosis — within one to two weeks.