What Is Sleep Apnea? Causes, Types, and Why It Matters
Sleep apnea causes repeated breathing pauses during sleep, affecting an estimated 936 million people worldwide. Learn how it works, who gets it, and why treatment matters.
Reviewed by Dr. Andrew Gamache, DDS, D-IAOS
Last updated February 2026
Key Takeaways
- Sleep apnea causes your airway to collapse repeatedly during sleep — often 30 or more times per hour — triggering oxygen drops, stress hormone surges, and sleep fragmentation that more time in bed cannot fix
- An estimated 936 million people worldwide have obstructive sleep apnea, yet roughly 80% of moderate-to-severe cases remain undiagnosed because the most damaging events happen during sleep
- Sleep apnea is a treatable condition with options including CPAP, oral appliance therapy, and lifestyle modifications — the critical first step is a proper diagnosis through a sleep study
Understanding Sleep Apnea
You have probably heard the term "sleep apnea" — maybe from a doctor, a partner who noticed something alarming while you slept, or an article that made you wonder whether your exhaustion has a medical explanation. Whatever brought you here, you deserve a clear answer, not jargon.
Sleep apnea is a condition where your breathing repeatedly stops and restarts during sleep. These pauses — called apneas — can last 10 seconds or longer and may happen dozens or even hundreds of times per night. Each time your breathing stops, your blood oxygen drops, your brain sends an emergency arousal signal, and your body shifts out of deep, restorative sleep. You rarely wake up enough to remember it. But your body remembers.
The result is a pattern that millions of people recognize: you go to bed, you appear to sleep, and you wake up feeling like you never rested. The fatigue accumulates. The brain fog settles in. And because the disruption happens while you are unconscious, most people spend months or years blaming stress, aging, or poor sleep habits before discovering the real cause.
People Affected Worldwide
Estimated global prevalence of obstructive sleep apnea according to Lancet Respiratory Medicine research
Cases Undiagnosed
Proportion of moderate-to-severe obstructive sleep apnea cases that remain undiagnosed in the US
Americans with OSA
Estimated number of US adults living with obstructive sleep apnea, most without knowing it
How Sleep Apnea Works: The Airway Mechanism
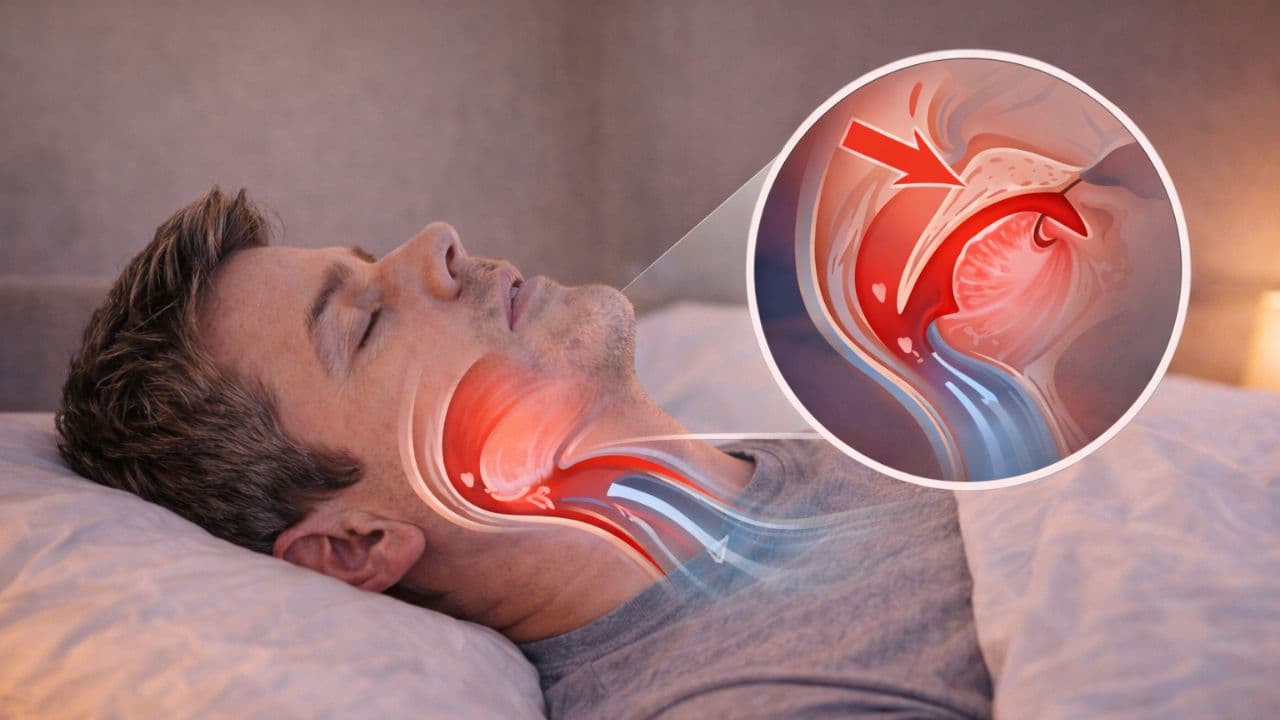
To understand sleep apnea, you need to understand what happens inside your airway every time you fall asleep. During waking hours, the muscles surrounding your throat keep your airway open. When you sleep, those muscles relax — and for people with sleep apnea, they relax too much, allowing the soft tissue to collapse inward and block airflow.
This sets off a cascade of physiological events that repeat throughout the night. Here is what a single apnea episode looks like from the inside:
Muscle Relaxation
As you enter deeper sleep stages, the muscles in your tongue, soft palate, and throat walls lose tone. The airway narrows progressively.
Airway Collapse
The relaxed tissue collapses inward, partially or completely blocking the airway. Airflow stops — this is the apnea. A partial collapse (hypopnea) reduces airflow by 30% or more.
Oxygen Drops
Without airflow, blood oxygen saturation falls. Drops from a normal 95-100% down to 80% or lower are common in severe cases, starving organs and tissues of oxygen.
Brain Emergency Signal
Your brain detects the oxygen crisis and triggers a stress response — releasing adrenaline and cortisol, spiking your heart rate, and sending a micro-arousal signal to restart breathing.
Brief Arousal and Recovery
You shift to a lighter sleep stage just long enough to restore muscle tone and reopen the airway. You gasp, snort, or shift position. Normal breathing resumes — briefly.
The Cycle Repeats
As you drift back toward deep sleep, muscle tone drops again, and the cycle restarts. In severe cases, this happens 30-60+ times per hour — preventing your body from ever reaching the restorative deep sleep it needs.
This cycle explains why sleep apnea causes so much damage despite appearing, on the surface, like ordinary sleep. Your body spends the night cycling through oxygen deprivation and stress hormone surges instead of cycling through the deep and REM sleep stages that restore memory, regulate hormones, and repair tissue. If you have been wondering why you feel exhausted despite sleeping 8 hours, this mechanism is often the answer.
The Three Types of Sleep Apnea
Not all sleep apnea is the same. While the symptoms often overlap, the underlying cause differs — and that distinction affects which treatments work best.
| Type | Cause | Prevalence | Key Treatment |
|---|---|---|---|
| Obstructive (OSA) | Physical airway collapse from relaxed throat muscles and soft tissue | 84% of cases | CPAP, oral appliances, positional therapy, surgery |
| Central (CSA) | Brain fails to send proper breathing signals to respiratory muscles | ~1% of cases | Adaptive servo-ventilation, treating underlying condition |
| Complex/Mixed | Combination of airway obstruction and central signaling failure | ~15% of cases | BiPAP or ASV therapy, combination approaches |
Obstructive sleep apnea is by far the most common type and the focus of most sleep apnea treatment, including oral appliance therapy. When people say "sleep apnea" without qualification, they almost always mean OSA. Central sleep apnea is relatively rare and typically associated with heart failure, opioid use, or neurological conditions. Complex sleep apnea sometimes emerges when a patient starts CPAP and the obstructive events resolve but central events appear.
Who Gets Sleep Apnea: Risk Factors
Sleep apnea does not discriminate as much as people think. While certain factors increase risk significantly, this condition affects people across every age group, body type, and demographic. The stereotype of the overweight, middle-aged man misses a large portion of the affected population — particularly women, who are underdiagnosed at alarming rates.
Excess Weight
Fat deposits around the upper airway narrow the breathing passage. A BMI above 30 is present in 60-90% of OSA patients. However, 20-40% of people with OSA are not overweight — anatomical factors play an equal role for many.
Neck Circumference
A neck circumference greater than 17 inches in men or 16 inches in women significantly increases risk, regardless of overall weight. A thick neck can compress the airway even in people with normal BMI.
Age Over 40
OSA prevalence increases significantly after age 40 and again after 60, as throat muscles lose tone with aging. Estimates suggest 20-30% of adults over 65 have at least mild OSA.
Male Sex (but Women Are Underdiagnosed)
Men are diagnosed roughly 2-3 times more often than women — but this gap narrows significantly after menopause. Women with OSA often present with different symptoms (fatigue, insomnia, depression) that lead to misdiagnosis.
Anatomical Factors
A recessed jaw (retrognathia), large tongue, enlarged tonsils, deviated septum, or naturally narrow airway all increase risk. These structural factors explain why some lean, fit, young adults develop sleep apnea.
Family history also plays a role. If a parent or sibling has sleep apnea, your risk increases — not just because of shared genetics affecting airway anatomy, but because of shared lifestyle and environmental factors.
Recognizing the Signs
Sleep apnea is tricky because its most obvious symptoms happen while you are asleep. The person lying next to you may notice snoring, gasping, or breathing pauses long before you suspect anything is wrong. But there are waking symptoms too — patterns that slowly become your normal without you realizing they are not.
Common Signs of Sleep Apnea:
If you recognize three or more of these signs, it is worth exploring further. Many people are surprised to learn that symptoms they attributed to stress, aging, or poor sleep habits actually have a treatable medical explanation. Our free sleep assessment can help you understand your risk in about two minutes.
Why Treatment Matters: Health Consequences
Sleep apnea is not "just snoring" or "just tiredness." The nightly cycle of oxygen deprivation and stress hormone surges creates measurable damage across multiple organ systems. The longer OSA goes untreated, the more these effects compound — which is why understanding the consequences of untreated sleep apnea matters.
Health Risks of Untreated Sleep Apnea:
These risks are not abstract. Research published in the American Journal of Respiratory and Critical Care Medicine found that untreated severe sleep apnea is associated with a significantly reduced life expectancy compared to treated patients. The good news is that effective treatment can reduce or reverse many of these risks — the body has a remarkable capacity to heal when restorative sleep is restored.
Getting Diagnosed and Treated
If you suspect sleep apnea, the path forward is more straightforward than most people expect. Diagnosis starts with a sleep study — which can often be done at home with a portable monitor — and your results will include an AHI score that classifies your severity.
Diagnosis Options:
Treatment Options:
The right treatment depends on your severity level, anatomy, lifestyle, and personal preferences. CPAP remains the gold standard, particularly for severe cases. But for patients with mild-to-moderate OSA — or those who have struggled with CPAP compliance — oral appliance therapy offers an effective, comfortable alternative with compliance rates exceeding 80%.
The most important step is the first one: getting tested. Sleep apnea does not improve on its own, but it is one of the most treatable conditions in sleep medicine. Understanding what it is — and recognizing it in your own experience — is where the path to better sleep begins.
Frequently Asked Questions
Is sleep apnea the same as snoring?
No. Snoring is vibration of soft tissue and can occur without sleep apnea. Sleep apnea involves actual cessation of breathing — the airway fully or partially closes, cutting off airflow for 10 seconds or more. However, loud, irregular snoring with pauses is one of the most common indicators that sleep apnea may be present.
Can young, healthy people get sleep apnea?
Yes. While obesity and age are major risk factors, sleep apnea also occurs in young, fit adults due to anatomical factors like a narrow airway, recessed jaw, or enlarged tonsils. Studies suggest 9-15% of adults aged 30-49 have at least mild OSA, regardless of weight.
How is sleep apnea different from insomnia?
Insomnia is difficulty falling or staying asleep. Sleep apnea is a breathing disorder that disrupts sleep quality even when you sleep through the night. Many sleep apnea patients do not have trouble falling asleep — they have trouble getting restorative sleep because their breathing is interrupted repeatedly.
Can sleep apnea go away on its own?
Sleep apnea rarely resolves without intervention. Significant weight loss (10-15% of body weight) can reduce AHI by up to 50%, but anatomical and age-related factors typically persist. Most patients need ongoing treatment — whether CPAP, an oral appliance, or another approach — to manage their condition effectively.